Drug Interactions: What You Need to Know Before Mixing Medications
If you’ve ever wondered why your doctor warns about taking certain pills together, you’re not alone. A drug interaction happens when two (or more) substances affect each other’s performance in the body. The result can be a weaker effect, stronger side‑effects, or even a serious health risk. Knowing the basics helps you avoid surprises and stay in control of your treatment.
Why Interactions Matter
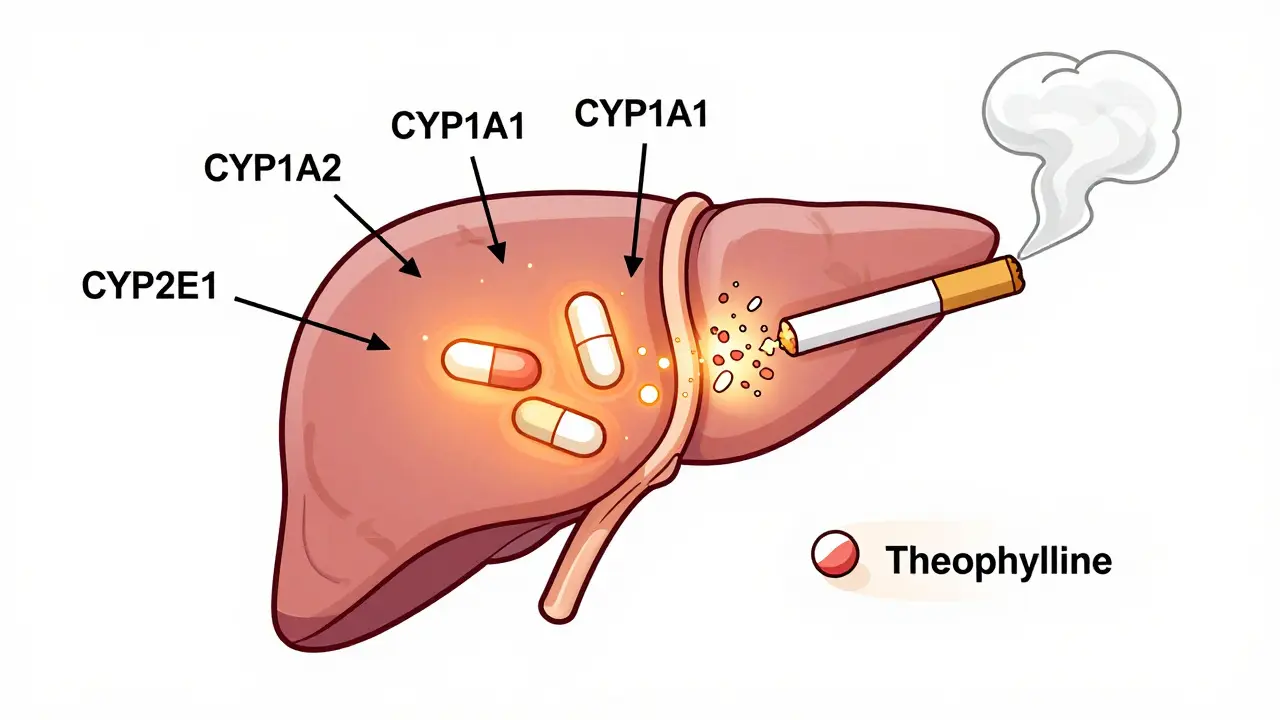
Every medication has a specific way it’s broken down—usually by liver enzymes called CYP450. When another drug uses the same pathway, they can compete, causing one to build up while the other disappears too fast. For example, taking an over‑the‑counter antihistamine with a prescription sleep aid might make you drowsy longer than expected. On the flip side, some antibiotics speed up heart medication breakdown, leaving your blood pressure higher than intended.
Simple Ways to Check Interactions
The easiest method is a drug interaction checker. Most pharmacy websites and health apps let you type in the names of all your meds, supplements, and even herbal products. The tool flags high‑risk combos and offers a short note on what might happen.
- Start with prescription labels: Write down every pill, dose, and how often you take it.
- Add OTCs and supplements: Pain relievers, vitamins, herbal teas—everything counts.
- Run the list through a checker: Look for red warnings (danger) and yellow ones (caution).
If you see a warning, don’t panic. Talk to your pharmacist or doctor right away. They can often switch one drug, adjust the dose, or suggest timing changes that keep everything safe.
Here are three common interaction scenarios you might recognize:
- Blood thinners + NSAIDs: Mixing ibuprofen with warfarin raises bleeding risk. Use acetaminophen instead if you need pain relief.
- Statins + certain antibiotics: A drug like clarithromycin can boost statin levels, leading to muscle pain. Your doctor may pause the statin during a short antibiotic course.
- SSRIs + migraine meds: Combining an SSRI antidepressant with triptans (e.g., sumatriptan) can increase serotonin syndrome chances. Monitoring is key.
Remember, food can act like a drug too. Grapefruit juice, for instance, blocks the same liver enzymes many cholesterol meds use, raising their concentration. A quick look at your medication guide will tell you if any foods need to be avoided.
When you get a new prescription, ask these three questions:
- Will this interact with anything I’m already taking?
- Do I need to change the time of day I take it?
- Are there foods or drinks I should steer clear of while on this drug?
Most doctors expect you to ask—it's a sign you’re taking your health seriously.
Finally, keep an updated medication list in one place. A simple note app on your phone works great, and you can show it to any healthcare provider during appointments. Updating the list whenever you start or stop a product keeps the interaction checks accurate.
Drug interactions might sound scary, but with a few habits—checking combos early, asking questions, and keeping records—you can protect yourself without extra hassle. Stay aware, use free online checkers, and let your pharmacist be part of the safety net.